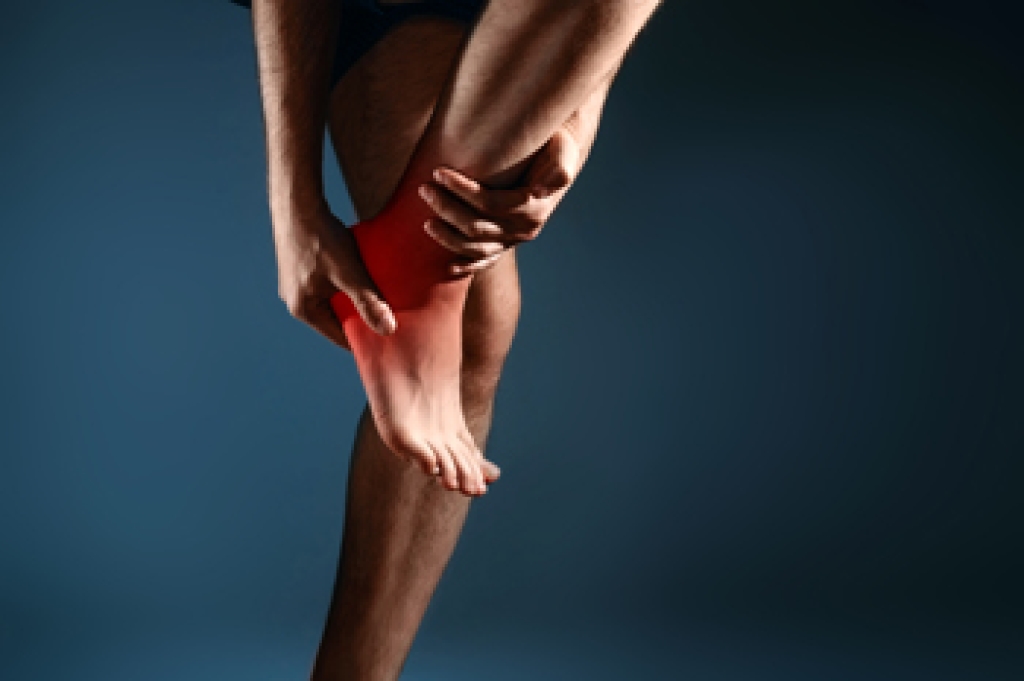
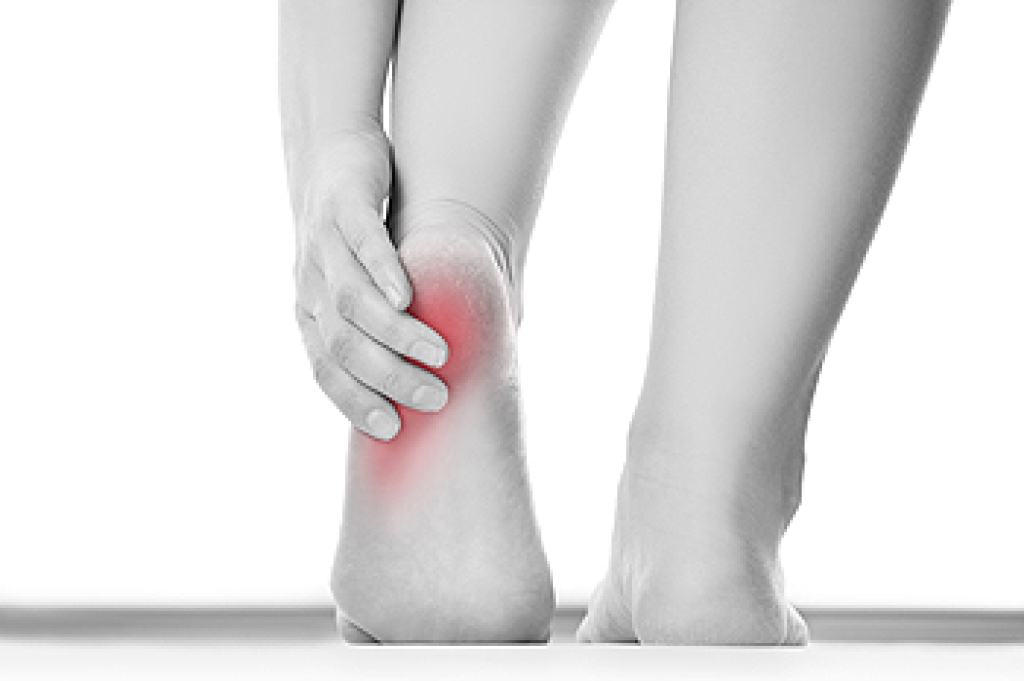
Ankle sprains are one of the most common injuries to occur during sports. Ankle sprains develop when ligaments that connect the bones in the foot, ankle, or lower leg become stretched or torn. This generally takes place when the ankle twists or rolls inwards and causes the ligaments on the outside of the ankle to over-stretch. Common signs of a sprained ankle include swelling that may be accompanied with a bruise, pain, a snap or cracking sound at the time of injury, and difficulty walking or bearing weight. Most ankle sprains are treated with rest, ice, anti-inflammatory medicines, and additional support for the ankle. However, because the symptoms of an ankle sprain are very similar to those of a broken ankle, patients who may have endured a sprained ankle should consult with a podiatrist for a proper diagnosis. A podiatrist will be able to make suggestions in order to prevent a recurring ankle sprain and provide a treatment technique that is specific to you.
Ankle sprains are one of the most common injuries to occur during sports. Ankle sprains develop when ligaments that connect the bones in the foot, ankle, or lower leg become stretched or torn. This generally takes place when the ankle twists or rolls inwards and causes the ligaments on the outside of the ankle to over-stretch. Common signs of a sprained ankle include swelling that may be accompanied with a bruise, pain, a snap or cracking sound at the time of injury, and difficulty walking or bearing weight. Most ankle sprains are treated with rest, ice, anti-inflammatory medicines, and additional support for the ankle. However, because the symptoms of an ankle sprain are very similar to those of a broken ankle, patients who may have endured a sprained ankle should consult with a podiatrist for a proper diagnosis. A podiatrist will be able to make suggestions in order to prevent a recurring ankle sprain and provide a treatment technique that is specific to you.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact Cary Golub, DPM from New York. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
- Pain at the sight of the tear
- Bruising/Swelling
- Ankle area is tender to touch
- In severe cases, may hear/feel something tear
- Skin discoloration
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact our offices located in Williston Park, and Long Beach, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.