Bunions are a foot condition where the big toe points toward the second toe, causing a bony bump to form at the base of the toe. They are particularly common in older women, anyone with flat feet, or people with a family history of bunions. Pregnancy can also contribute, as hormonal changes and weight gain put additional pressure on the feet. Symptoms of bunions include pain, swelling, and redness surrounding the joint, often worsened by wearing tight or narrow shoes. As the condition progresses, it can lead to difficulty walking and discomfort during daily activities. A podiatrist can diagnose the severity of the bunion and offer treatment options to reduce pain and slow progression. Conservative options include custom orthotics, padding, or changes to footwear. In more severe cases, surgery may be needed to realign the toe. If you have a bunion, it is suggested that you schedule an appointment with a podiatrist for proper treatment.
If you are suffering from bunion pain, contact Cary Golub, DPM of New York. Our doctor can provide the care you need to keep you pain-free and on your feet.
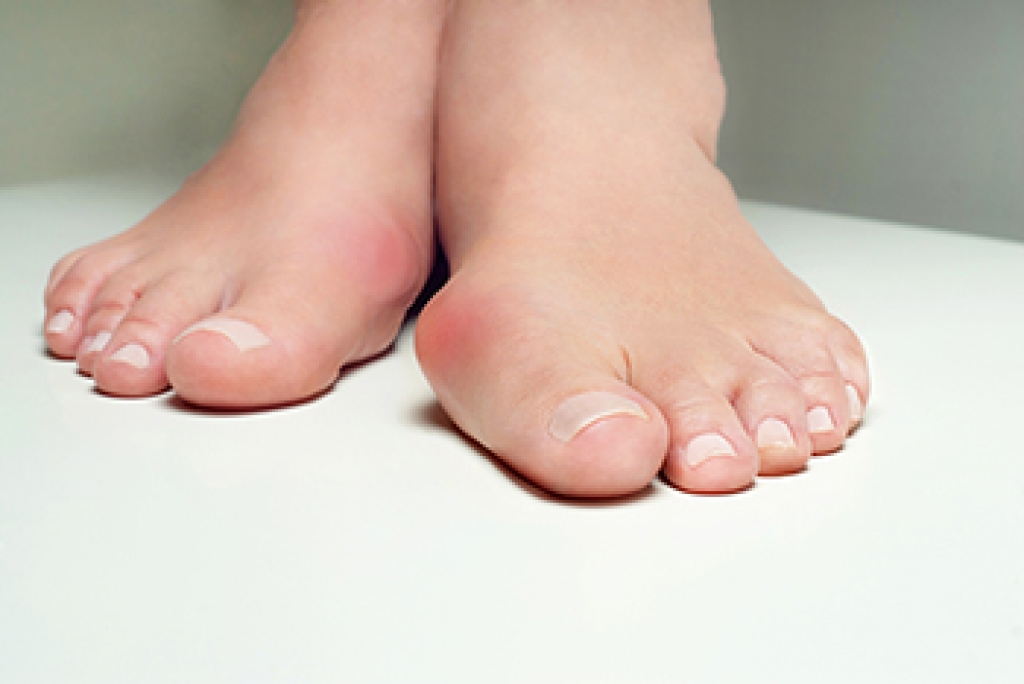
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Williston Park, and Long Beach, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.